
Each May, Mental Health Awareness Month turns a spotlight on clinician well-being. In 2026, that light lands on a workforce showing positive, if uneven, improvement — and a set of structural problems that awareness campaigns alone cannot fix. Physician burnout has edged down for the fourth consecutive year, with 41.9% of physicians reporting at least one symptom in 2025, down from 43.2% in 2024 and 48.2% in 2023. American Medical Association
The headline from this year’s data is cautiously optimistic. The AMA’s 2025 National Physician Comparison Report, drawn from nearly 19,000 responses across 38 states and 106 health systems, found that both job stress and burnout continued to decline — by 2.2 and 1.3 percentage points respectively. The share of physicians who reported feeling valued rose to 56.2%. Intent to leave within two years ticked down to 31.1%.
But aggregate improvements can obscure what’s truly happening at the front lines.
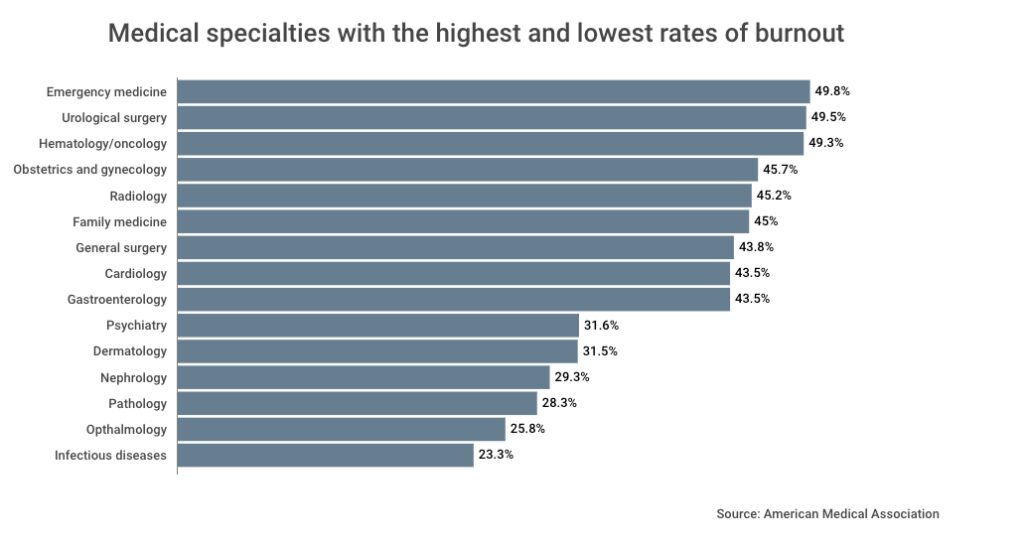
Emergency medicine, urological surgery, and hematology/oncology reported the highest burnout rates, all approaching or exceeding 49%.
A separate analysis published this spring noted that Medscape’s most recent Physician Burnout and Depression Report put the overall figure at 62% — with “too much bureaucratic work” and electronic health records ranking as the top two contributors for the second year running. Nearly one in four physicians surveyed said they are planning to leave clinical medicine within the next few years because of it.
The divergence between data sources reflects how burnout is measured and who gets counted. What they agree on is the problem has not been solved, and it is not distributed evenly.
Physician burnout is frequently framed as a profession-wide challenge. The data suggests it is more usefully understood as a geography of pressure — concentrated in the roles, settings, and regions where operational strain is highest and flexibility is lowest.
In contrast to high-burnout specialties like emergency medicine and hematology/oncology, infectious diseases (23.3%), nephrology (29.3%), and dermatology (31.5%) reported significantly lower rates. The gap between the top and bottom of that range spans more than 25 percentage points. That is not a difference in individual resilience, but rather a difference in how those jobs are structured.
Emergency physicians and hospitalists face a specific combination: high patient volume, unpredictable surges, shift-based schedules, and boarding constraints that extend well beyond their department. These are not roles on the periphery of hospital operations. They sit at the center of access, patient flow, and revenue. When coverage falters, the effects are immediate: shifts extend, recovery windows shrink, and the remaining workforce absorbs the gap.
Recent data reinforces the downstream workforce risk. In Virginia, more than one in four primary care clinicians reported intent to reduce clinical hours over the next year — 29.7% of APPs and 28.4% of physicians in primary care specifically. Vahealthinnovation
While patient-facing intensity draws the most attention, the paperwork side of medicine continues to impose its own quiet tax.
Research consistently finds that for every hour of patient care, physicians spend nearly two additional hours on administrative tasks — primarily EHR documentation. That ratio has proven stubbornly resistant to reform. A study of primary care physicians at Massachusetts General and Brigham and Women’s hospitals found that a typical 30-minute scheduled visit generated 36.2 minutes of EHR time — including 6.2 minutes of “pajama time” completed after 5:30 p.m. arxivAmerican Medical Association
AMA survey data shows that 20.9% of physicians spent more than eight hours per week on the EHR outside normal work hours — the same figure as in 2022. Despite years of attention to the problem, pajama time has not moved. American Medical Association
There is early evidence, however, that AI-assisted documentation may change the equation. A 2025 study in JAMA Network Open found that after 30 days using an ambient AI scribe, burnout among ambulatory clinicians dropped from 51.9% to 38.8%, with significant improvements in after-hours documentation time and cognitive task load. That is a single intervention in controlled conditions — but it points toward where leverage may exist. PubMed Central
Burnout does not occur in a vacuum. It is amplified when it collides with a shrinking supply of available clinicians.
The AAMC projects the United States will face a physician shortage of up to 86,000 by 2036, driven primarily by population growth and the rapid aging of both patients and the physician workforce itself. Physicians aged 65 and older currently make up 20% of the clinical workforce, with another 22% between 55 and 64 — a substantial portion approaching retirement age simultaneously. AAMCAAMC
Shortages rarely show up as vacant positions on a job board. In practice, they redistribute. Clinicians pick up additional shifts. Hours lengthen. Recovery time compresses. The burden concentrates on whoever remains, and the cycle compounds.
Nearly half of U.S. physicians report working with inadequately staffed teams, a condition associated with significantly higher odds of burnout and increased intent to leave the profession (American Medical Association, 2023; Mayo Clinic Proceedings).
Beyond workload, a second variable appears consistently across burnout research: autonomy. Specifically, control over when and how work gets done.
The AMA identifies lack of schedule control as one of the primary structural drivers of burnout. Research published in Mayo Clinic Proceedings has found that physicians with greater scheduling flexibility consistently report higher job satisfaction and lower burnout rates, even when total hours worked are similar. In environments where patient demand, regulatory requirements, and payer rules are largely fixed, time remains one of the few variables that can actually be adjusted.
The implication for hospital-based specialties is straightforward. Locum and flexible staffing arrangements, shift-based employment with genuine flexibility, and models that give clinicians meaningful input into their schedules have measurable effects on how that workload is experienced, even when the workload itself doesn’t change.
Healthcare organizations have invested significantly in wellness programming, resilience training, and mental health resources. Many of these initiatives accelerate in May. The aggregate data, however, has not kept pace with that investment.
A review published in The Lancet found that while individual-focused interventions can produce short-term benefit, organizational changes — workflow redesign, staffing improvements, administrative reduction — produce more sustained outcomes.
Even the AMA, which has reported four consecutive years of declining burnout, cautions against declaring victory. Systemic challenges remain, and the data underscores the need for continued structural change. American Medical Association
Mental Health Month has succeeded in normalizing the conversation. The question it has not yet answered is whether awareness, absent operational change, can sustain the improvement that’s begun.
Studies published in JAMA, Mayo Clinic Proceedings, and The Lancet point toward a consistent set of interventions with meaningful impact:
The pattern across datasets is clear: interventions that target workload and control produce the most durable results.
The 2025 data offers something that has been scarce in this conversation for years: genuine evidence of improvement. Burnout is down from its post-COVID peak. Physician satisfaction has held steady. Health systems that invested in well-being infrastructure are seeing returns.
But nearly 42% of physicians still report burnout symptoms. Emergency medicine still sits above 49%. The physician shortage is accelerating. Pajama time hasn’t moved in three years. And one in four physicians is considering leaving clinical medicine.
Mental Health Month is a useful frame. It is not, by itself, a solution. The data has been pointing in the same direction for a decade: the clinicians who are most burned out are the ones operating with the least margin, the least control, and the least flexibility. Addressing that requires changes at the operational level, not just the awareness level.
The AMA’s most recent data puts physician burnout at 41.9% in 2025 — the lowest rate since before COVID-19. The Medscape Physician Burnout and Depression Report uses a broader definition and has reported higher figures, with 62% of physicians indicating burnout in their most recent survey. The gap reflects methodological differences, not contradiction. American Medical AssociationKevinMD
Emergency medicine, urological surgery, and hematology/oncology lead national rankings, all approaching or exceeding 49% in the AMA’s 2025 data. Healthcare IT News
Bureaucratic workload and EHR demands are the top two drivers, according to Medscape, cited by 62% of physicians reporting burnout. Staffing shortages, limited schedule control, and long hours round out the picture. KevinMD
Better, by most measures — but unevenly. Aggregate rates have declined for four consecutive years, while certain specialties and care settings remain well above the national average, and structural drivers like administrative burden and workforce shortages have not materially improved.
The strongest evidence points to organizational-level changes: improved staffing coverage, workflow redesign, reduced administrative burden, and greater schedule flexibility. Individual wellness programs help, but the research base consistently finds larger and more durable effects from structural interventions.