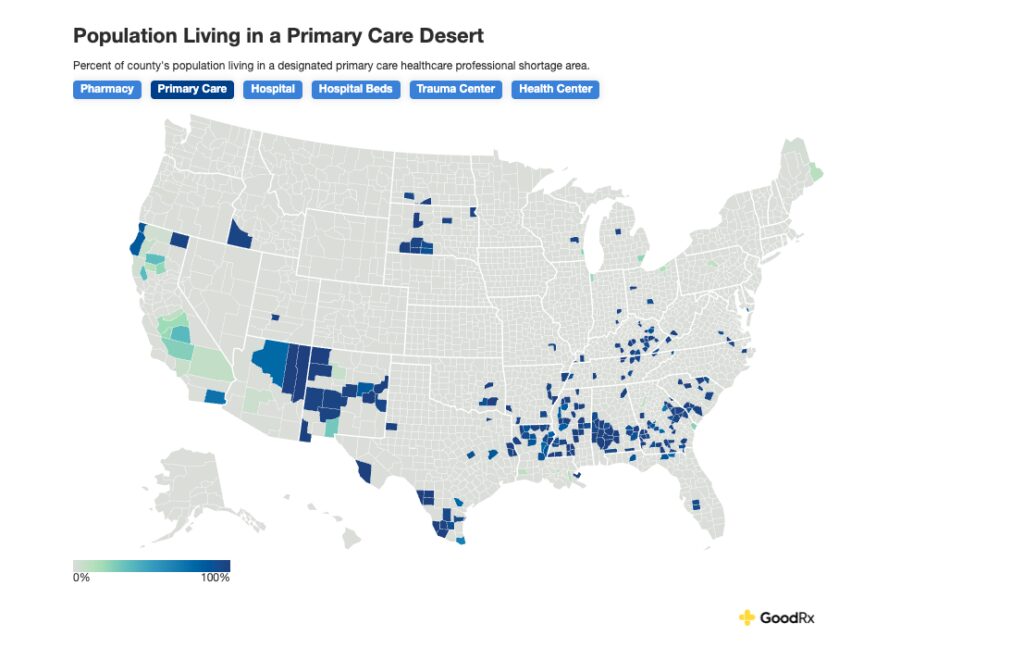
In more than 80 percent of U.S. counties, access to essential healthcare services is limited. According to research from GoodRx, more than 120 million Americans, roughly one in three people, live in a healthcare desert. These are communities where access to primary care, pharmacies, hospital beds, or trauma services is constrained or out of reach.
The primary care physician shortage looks like a waiting room that never empties. It sounds like a front desk explaining, again, that the next available new patient appointment is six weeks out. It feels like a rural health system CEO watching access metrics soften while recruitment stretches into its fifth month.
The United States is not drifting toward a primary care crisis. It is already living it.
The Data Behind the Primary Care Physician Shortage
The pressure begins with demographics.
The U.S. population aged 65 and older is projected to grow by roughly 42 percent, rising from 58 million in 2022 to more than 82 million by 2050. By 2034, older adults are expected to outnumber children. That shift alone changes the demand curve. Older adults use primary care at significantly higher rates and often manage multiple chronic conditions that require ongoing, longitudinal care.
Now place that demand curve against workforce reality.
- According to the Health Resources and Services Administration, the country needs more than 17,000 additional primary care practitioners today just to eliminate existing shortages.
- The Association of American Medical Colleges projects a shortage of up to 48,000 primary care physicians by 2034.
- A 2024 analysis from the National Center for Health Workforce Analysis estimates that gap could widen to more than 87,000 full-time equivalent primary care physicians by 2037.
Demand is accelerating. Unfortunately, the pipeline is not.
And the access problem extends beyond headcount.
In designated primary care deserts, home to nearly 8 million people, there is just one full-time primary care professional for every 7,597 residents. That is more than 2.5 times the recommended ratio.
This is not a narrow rural issue. It is a structural access problem embedded across the country, where demand is rising, supply is thinning, and geography compounds the strain.
Primary Care Wait Times: The First Visible Sign of the Physician Shortage
When workforce strain intensifies, access to care is the first system to show it.
National appointment surveys in major metropolitan areas report average new patient primary care wait times exceeding three weeks. In rural markets, delays often stretch beyond 30 to 60 days. In some communities, the only alternative is a long drive or the emergency department.
Layer that against the GoodRx data and the picture sharpens. In counties already classified as healthcare deserts, limited provider supply and long travel distances compound scheduling delays.
A missed hypertension follow-up becomes an ED visit. A delayed colorectal cancer screening becomes a late-stage diagnosis. A deferred diabetes check-in becomes an avoidable hospitalization.
Strong primary care keeps people out of the emergency department and out of the hospital. It catches problems early, manages chronic disease consistently, and keeps preventive care on track. On the flip side: when access shrinks, small issues escalate, emergency visits rise and hospital admissions increase.
The State-Level Reality
The shortage has geography, and the response varies by state.
In Michigan, projections suggest the state could be short at least 800 primary care physicians by 2030. Policymakers are pursuing scope-of-practice reforms to expand nurse practitioner autonomy in response. It is a meaningful step, but legislation moves slower than patient demand, and health systems must bridge access gaps in the meantime.
In Maine, the pressure is demographic. The state is projected to face a shortage of roughly 120 primary care physicians by 2030. Nearly one-third of Maine’s primary care doctors are age 60 or older, positioning retirement as a defining force over the next decade. Residency expansion is part of the strategy, yet in-state training capacity remains limited and many graduates practice elsewhere.
In rural Arizona, leaders are investing in the pipeline. Onvida Health and the University of Arizona College of Medicine–Phoenix launched the state’s first rural regional medical school branch in Yuma County. Beginning 2026, 15 students annually train through an accelerated primary care pathway with full tuition scholarships funded locally.
Each of these states is working on long-term structural change. But, unfortunately, long-term solutions do not fill next month’s schedule.
Rural Healthcare: When One Vacancy Changes Everything
In rural America, primary care is not just a service line. It is a health infrastructure.
Rural counties represent nearly one in five Americans yet have significantly fewer physicians per capita. Many communities rely on a single clinic or critical access hospital.
When one primary care physician leaves, capacity can drop by 25 to 50 percent overnight.
Federally Qualified Health Centers: Access Under Compliance Pressure
Federally Qualified Health Centers sit at the center of the primary care access crisis.
According to the Health Resources and Services Administration, health centers serve more than 30 million patients annually, the majority of whom are uninsured or covered by Medicaid. These organizations operate under strict federal reporting requirements and quality benchmarks tied directly to funding.
That structure creates a narrow margin for workforce instability. When a primary care vacancy opens inside an FQHC, the impact is immediate and measurable. Preventive screening rates decline. Chronic disease management metrics soften. Appointment availability tightens. Panels redistribute. Staff absorb more volume. Morale shifts.
Unlike larger systems, many FQHCs do not have deep bench capacity to absorb sustained gaps.
At the same time, the broader primary care market is under financial pressure. As reported by NPR, independent primary care physicians are increasingly consolidating into Independent Physician Associations to manage reimbursement volatility and Medicaid uncertainty. That consolidation trend reflects a deeper reality: financial fragility and workforce fragility often move together.
Demand does not pause while payment models evolve. Chronic disease does not wait for recruitment cycles to close. For FQHC leaders, access stability is not optional. It is tied directly to compliance, funding, and community trust.
Locum Tenens: Stability While the System Rebuilds
Locum tenens is often described as temporary coverage. In the current workforce and healthcare desert environment, it is access preservation.
Strategic deployment can maintain appointment availability, prevent panel closures, protect preventive screening rates, stabilize chronic care management metrics, and reduce emergency department spillover.
In rural systems and FQHCs, locum tenens buys time. Time to recruit thoughtfully, protect quality benchmarks and keep community trust intact.
Immediate Scale When Access Cannot Wait
For organizations confronting immediate primary care access gaps, scale matters.
Barton Associates currently has:
- Primary care locums in every U.S. state., with strongest presence in California, Florida, Texas, New York, North Carolina, Pennsylvania, New Jersey, Georgia, Michigan and Arizona.
- Barton’s broader provider network includes over 6,000 credentialed primary care clinicians, including MDs, DOs, NPs, and PAs.
That represents deployable capacity across family medicine, internal medicine, and advanced practice primary care coverage nationwide.
In a country where more than 120 million people live in healthcare deserts and over 80 percent of counties face some form of access limitation, immediate coverage is not a luxury. It is stabilization.
The primary care shortage is structural. The healthcare desert map is already drawn. Communities need continuity now.
And in many towns across Michigan, Maine, Arizona, and beyond, the waiting room is already full.



